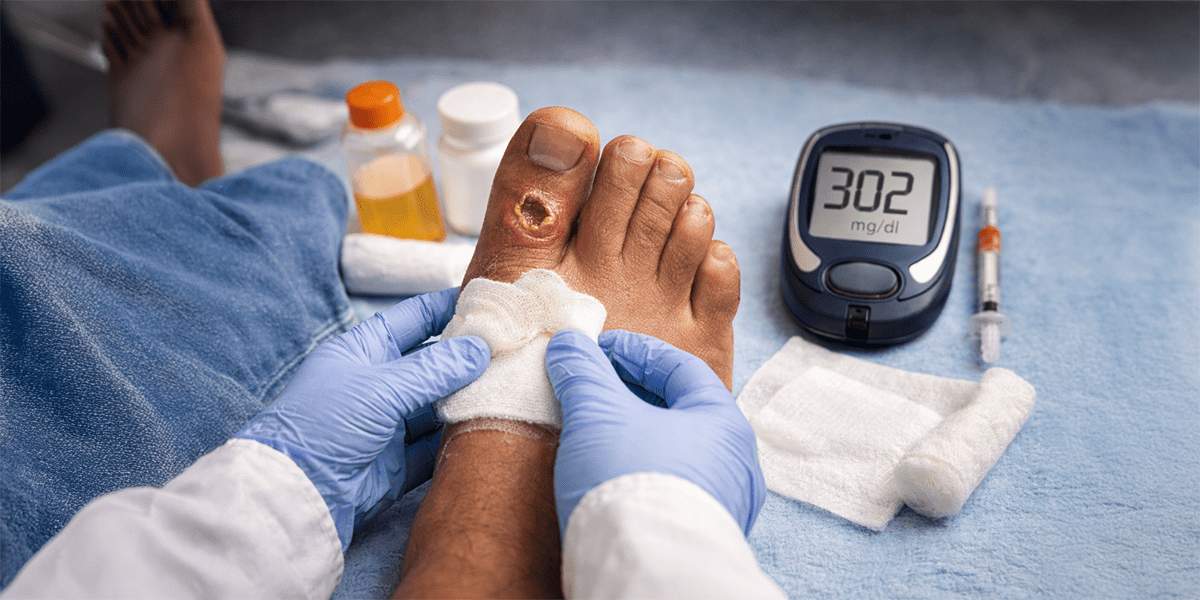
Under normal conditions, wound healing follows a predictable sequence of inflammation, tissue formation, and remodeling. In individuals with diabetes, this process may be disrupted. Chronic hyperglycaemia affects blood vessels, nerves, immune function, and collagen synthesis. Elevated blood glucose impairs white blood cell activity, reducing the body’s ability to fight infection. It also damages small blood vessels, limiting oxygen and nutrient delivery to injured tissue (Armstrong et al., 2017).
Peripheral neuropathy, a common complication of long-standing diabetes, reduces sensation in the feet. Minor injuries may go unnoticed, allowing them to worsen before treatment is initiated. In addition, peripheral arterial disease reduces blood flow, further delaying tissue repair. These factors combined explain why diabetic wounds, particularly foot ulcers, require prompt and structured care.
Diabetic foot ulcers are among the most serious complications of diabetes. They often begin as small areas of pressure or callus formation and may progress to deeper tissue involvement if untreated. Globally, diabetic foot ulcers are a leading cause of hospitalization and lower-limb amputation, early detection and intervention significantly reduce complication risk. Signs that require medical evaluation include persistent redness, swelling, warmth, discharge, foul odor, increasing pain, or wounds that do not show signs of improvement within two to four weeks.
Effective diabetic wound management requires a multidisciplinary approach. Blood glucose optimization is fundamental. Poor glycaemic control is strongly associated with delayed wound healing (American Diabetes Association, 2023). Offloading pressure from the affected area is critical, especially in foot ulcers. Special footwear or devices may be recommended to prevent further tissue damage.
Wound cleansing, debridement when necessary, infection control, and appropriate dressings are central to modern wound care. Moist wound environments using hydrocolloid, alginate, or foam dressings are often preferred depending on wound characteristics. In selected cases, advanced interventions such as negative pressure wound therapy or hyperbaric oxygen therapy may be considered under specialist supervision.
Adequate blood supply is essential for healing. Peripheral arterial disease must be evaluated in patients with chronic wounds. In some cases, vascular intervention may be necessary. Nutrition also plays a significant role. Protein deficiency, low micronutrient intake, and poor metabolic control can delay healing. Adequate protein, vitamin C, zinc, and overall caloric intake support collagen formation and tissue repair (Guo & DiPietro, 2010). Hydration and smoking cessation are equally important.
In Ayurveda, chronic non-healing wounds are described under Dushta Vrana. Classical texts emphasize cleansing, local wound care, and systemic balance. From an integrative standpoint, certain Ayurvedic external applications containing turmeric or neem have demonstrated antimicrobial and anti-inflammatory properties in laboratory studies (Gupta et al., 2017). However, these should only be used when wounds are medically evaluated and under professional supervision.
Ayurveda also emphasizes metabolic regulation, digestive balance, and lifestyle correction, which align with modern recommendations for glycaemic control and systemic inflammation reduction. It is essential to clarify that herbal or traditional applications should never replace medical debridement, antibiotics when indicated, vascular assessment, or specialist diabetic foot care.
Daily foot inspection remains one of the most effective preventive measures. Individuals with neuropathy should examine their feet regularly or seek assistance. Maintaining HbA1c within target range significantly reduces the risk of complications. Wearing appropriate footwear, trimming nails carefully, and avoiding walking barefoot are simple but effective preventive practices. Early consultation at the first sign of a wound can prevent progression to more severe stages.
Management of diabetic wounds requires collaboration between diabetologists, wound care specialists, vascular surgeons when necessary, nutritionists, and supportive care practitioners. Ayurvedic principles may contribute through dietary regulation, stress management, and carefully supervised topical or systemic herbal support in stable cases. However, they must be integrated responsibly within evidence-based medical care. The goal is not rapid cosmetic healing, but safe tissue repair, infection prevention, and limb preservation.
American Diabetes Association (2023). Standards of Medical Care in Diabetes. [LINK]
Armstrong, D.G. et al. (2017). Five year mortality and direct costs of care for people with diabetic foot complications. [LINK]
Guo, S. & DiPietro, L.A. (2010). Factors affecting wound healing. [LINK]
Gupta, S.C. et al. (2017). Therapeutic roles of curcumin: Lessons learned from clinical trials. [LINK]
This article is intended for educational purposes only and does not constitute medical advice. Diabetic wounds require prompt clinical evaluation. Delayed or inadequate treatment can lead to serious complications, including infection and amputation. Ayurvedic therapies should only be used under qualified supervision and must not replace standard medical wound care.